Pressure ulcers, more commonly called “bed sores”, represent a preventable and treatable issue for seniors, but caregivers must be vigilant to monitor for the potential of this malady. Further, these wounds can happen in places other than beds. They can appear and worsen very quickly so consistent and close inspections are important. Repositioning of those receiving care and consistent skin maintenance are critical.
Pressure ulcers occur when the blood supply is cut off to the area resulting in the tissue becoming injured and killing the flesh. This occurs when tissue is compressed between two relatively hard surfaces like the bone inside the body pressing against a bed or a chair. Older skin provides much less protection from injury than younger skin.
What Causes Bed Sores?
- Bed sores occur from pressure exerted from sitting or lying too long without shifting position. It is incumbent upon caregivers to be mindful of altering a senior’s position regularly. This is the most common cause of pressure ulcers.
- Skin can become abraded by dragging one’s body over bedsheets during transfers where friction or rubbing can occur. Being mindful of this possibility during the necessary relocation of a non-ambulatory individual will prevent unintended injury.
- Sliding in a chair or bed can create “shearing” where the skin slides or pulls away from the supportive tissue below it.
What are the at-risk areas?
The diagram below indicates the areas of most concern:
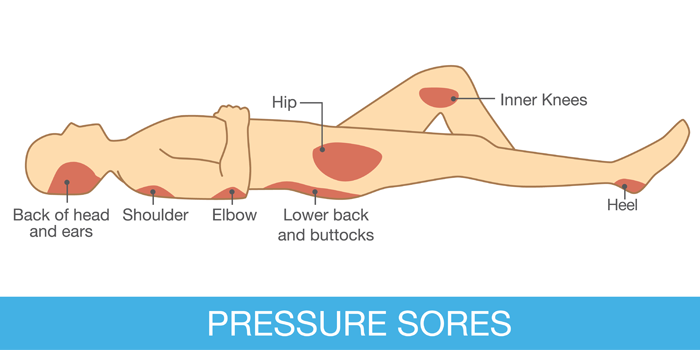
Careful observation is critical
Regular inspection of care recipients by both family and professional caregivers will reveal the first signs of pressure sores while the skin is still intact. Some signs that pressure sores may be an issue can be observed as follows:
- Changes in the color of the skin. Look for irritations which may manifest as blue or purple in darker skin or pink or red with those of lighter skin color.
- Skin temperature. When the skin is warm to the touch it indicates inflammation. Coolness indicates reduced blood flow to the area. Both situations are subject of concern.
- Tissue consistency. It is of concern when skin feels different from surrounding tissue. This can manifest as soft or “mushy”.
- Unusual sensation. Should the patient report pain, tingling, burning or itching in the at-risk areas it may indicate that a wound is developing.
- Minor wounds. Observation of small abrasions or blisters represent the type of superficial injuries that can become more serious quickly. Treat them immediately.
- Bruising. Bruising can occur after a fall. While it might look like a simple bruise, it should be carefully observed to make certain it does not turn into a sore. Deep bruises, particularly in at-risk areas, are more serious and can indicate substantial damage below the skin.
Preventing Bed Sores
While curing bed sores can be challenging, it is far better to prevent them altogether. A consistent regimen of preventative measures can accomplish this objective.
- Keep the skin lubricated and moisture free in risk areas.
- Perform daily skin checks of at-risk areas.
- Reposition the patient every two hours at a minimum.
- Provide extra cushioning for the at-risk areas.
- Include adequate protein, vitamins and minerals in meals.
Conclusion
Pressure sores that are not addressed quickly can become life-threatening infections. Delayed or improper care can lead to complications or additional wounds. Caregiver diligence should be part of a daily routine of inspection and quick response to signs of distress. Professional caregivers are trained to observe signs of pressure ulcers. Family caregivers must be equally aware.

